For many years, the time period “elective surgical procedure” merely meant a process that could possibly be scheduled upfront somewhat than an emergency that required an ambulance. It was a scheduling distinction, not a monetary one, and it included very important surgical procedures like joint replacements and cataract removals that improved a affected person’s high quality of life. Nonetheless, within the cost-containment panorama of 2026, insurance coverage firms have weaponized this definition to disclaim protection for procedures that docs deem medically crucial. By reclassifying practical repairs as “beauty” or “way of life enhancements,” payers are shifting the total monetary burden onto sufferers who are sometimes in vital ache.
This semantic shift permits insurers to bypass the protections of the Reasonably priced Care Act by claiming these providers fall outdoors the scope of “Important Well being Advantages.” Sufferers who’ve paid their premiums for years are shocked to seek out that the surgical procedure to repair their imaginative and prescient or their capability to stroll is now seen by their plan as a luxurious buy akin to a facelift. In case you are planning a surgical procedure this yr, you want to concentrate on the strict new “medical necessity” standards which may block your path. Listed below are seven medical providers thought of elective in 2026 that had been customary protection just some years in the past.
1. Higher Eyelid Lifts (Blepharoplasty)
As we age, the pores and skin of the higher eyelid can droop considerably, generally hanging so low that it bodily obstructs a senior’s imaginative and prescient and makes driving harmful. In earlier years, a easy “visible subject take a look at” displaying a 30% obstruction was sufficient to get Medicare or non-public insurance coverage to cowl the restore.
In 2026, the standards have tightened dramatically, with insurers typically requiring a 50% or higher obstruction that’s uncorrectable by tape or different non-surgical means. In line with American Academy of Ophthalmology advocacy alerts, claims for practical blepharoplasty are actually denied at a charge of practically 40% on the primary submission. Insurers are more and more categorizing this as a “beauty youth-enhancing process” whatever the affected person’s visible complaints, forcing seniors to pay the typical $5,000 value out-of-pocket to see the street clearly once more.
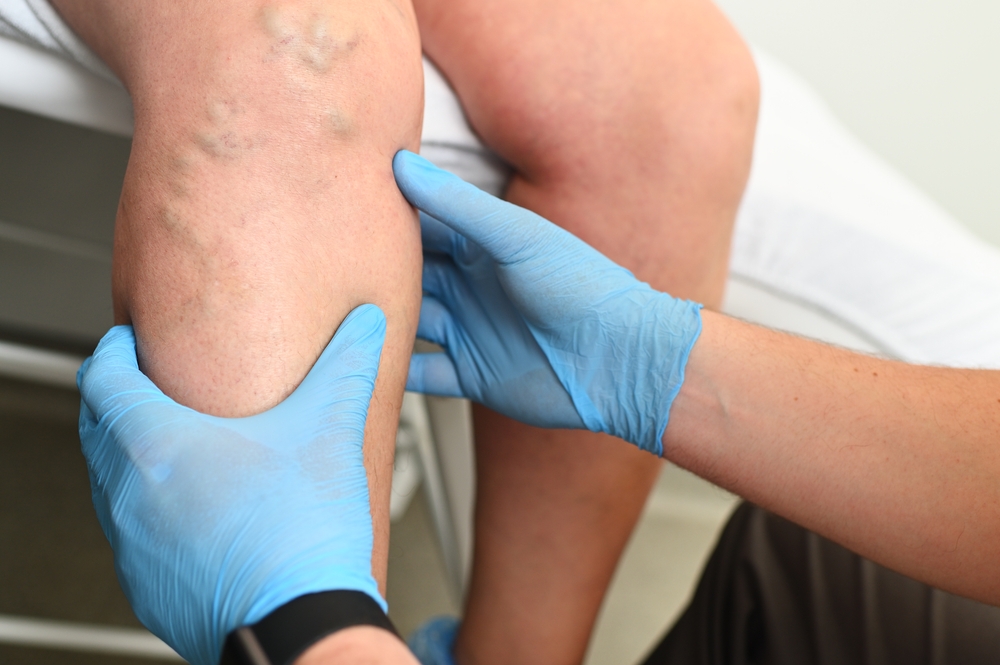
2. Varicose Vein Ablation
Varicose veins are sometimes dismissed as an arrogance concern, however for hundreds of thousands of Individuals, they trigger extreme leg heaviness, swelling, and painful ulcers that make engaged on one’s ft inconceivable. Traditionally, displaying “venous reflux” (backward blood stream) on an ultrasound was adequate to authorize laser ablation therapy.
Now, nearly each main payer has instituted a compulsory “Conservative Remedy” interval of six to 12 months earlier than they are going to even take into account surgical procedure. Sufferers should show they’ve worn prescription-grade compression stockings day by day for half a yr—and documented that they failed to supply aid—earlier than the surgical procedure is upgraded from “beauty” to “medically crucial.” For those who skip the stockings or lose the receipts proving to procure them, the $3,000 per leg process is taken into account strictly elective.
3. Pores and skin Removing After Weight Loss (Panniculectomy)
With the explosion of GLP-1 weight reduction medicine, hundreds of thousands of Individuals have misplaced huge quantities of weight quickly, resulting in extra pores and skin that may trigger extreme infections and mobility points. Insurers have responded to this wave of potential claims by creating practically inconceivable limitations for protection of a panniculectomy (eradicating the hanging pores and skin apron).
A 2026 overview of cosmetic surgery protection insurance policies signifies that sufferers should now present photographs of “intractable rashes” which have endured for 3 months regardless of prescription antifungal therapy. With out this graphic and steady documentation of pores and skin breakdown, the insurer classifies the surgical procedure as “physique contouring,” which is a contract exclusion in nearly each well being plan, leaving the affected person to pay $10,000 to $15,000 for aid.
4. Deviated Septum Restore (Septoplasty)
Many individuals are born with or develop a crooked nasal septum that blocks airflow, resulting in power sinus infections and sleep disruption. In 2026, insurers are conflating practical septoplasty with beauty rhinoplasty (nostril jobs) to disclaim claims. The brand new customary for “medical necessity” typically requires the affected person to show they’ve extreme Obstructive Sleep Apnea (OSA) and have failed CPAP remedy earlier than the surgical procedure is accredited.
Merely saying “I can’t breathe by my left nostril” is now not sufficient to set off protection. Until you’ll be able to produce a failed sleep examine and a yr of documented steroid spray use, the insurer will seemingly tag the surgical procedure as “elective nasal reshaping” and deny the $6,000 declare.
5. Arthroscopic “Clear-Up” Knee Surgical procedure
For many years, if a affected person had a torn meniscus and knee ache, the physician would go in with a scope to “clear up” the joint. In 2026, the medical consensus—and insurance coverage coverage—has shifted to view this as largely ineffective for arthritis sufferers.
Until there’s a “mechanical block” (the place the knee bodily locks up), insurers now classify arthroscopic debridement as an “elective” process with low worth. They successfully mandate six weeks of bodily remedy and cortisone injections as the first therapy. In order for you the surgical procedure with out leaping by these hoops, you’ll seemingly need to pay the ability price and surgeon’s price your self, because the payer views it as a placebo process for getting old knees.
6. Bariatric Revision Surgical procedure
Whereas preliminary weight reduction surgical procedure is broadly coated, “Revision Surgical procedure”—fixing or altering the abdomen years later on account of weight regain or issues—is going through a protection cliff. Insurers in 2026 are more and more classifying revisions as “elective conduct modification” somewhat than medical error correction.
They argue that if the affected person gained weight again, it’s a failure of way of life, not the system, and due to this fact a second surgical procedure shouldn’t be medically crucial. This leaves sufferers with extreme acid reflux disease or mechanical points from previous lap bands going through a $20,000 invoice to repair an issue that was initially coated by insurance coverage, just because the revision code is flagged as “investigational” or “lifestyle-based.”
7. “Early” Cataract Surgical procedure
Cataract surgical procedure stays the most typical process in Medicare, however the definition of when you’ll be able to have it has moved. Beforehand, if glare bothered you whereas driving at night time, you possibly can qualify for surgical procedure. In 2026, Medicare Benefit plans and business insurers are strictly implementing a “20/40 or worse” imaginative and prescient acuity rule or particular “Actions of Day by day Dwelling” (ADL) impairment scores.
In case your imaginative and prescient is 20/30 however you endure from horrible glare, the surgical procedure is taken into account “Refractive Lens Trade”—an elective imaginative and prescient correction just like LASIK. This forces sufferers to attend till their imaginative and prescient deteriorates considerably earlier than the “medical necessity” swap flips, or pay $4,000 per eye to have the process executed whereas they will nonetheless perform.
The “Conservative Remedy” Lure
The widespread thread connecting these reclassifications is the requirement for “Conservative Remedy.” In 2026, your insurance coverage firm needs you to strive a budget repair—stockings, nasal sprays, eye drops, or bodily remedy—for months earlier than they comply with the costly repair. The “elective” label is commonly momentary; you’ll be able to peel it off, however provided that you play their documentation recreation completely. Earlier than reserving any process that improves your high quality of life, ask your surgeon’s coordinator particularly: “What conservative remedy documentation does my plan require to show this isn’t elective?”
Have you ever been informed your medically crucial surgical procedure is “beauty” or “elective” this yr? Depart a remark under—your expertise helps others struggle these denials!
